Originally published in Issue 1 2005 icon
The Secret Weapon In Breast Cancer Detection?
By Madeleine Kingsley
Once upon a time, thermography was a secret weapon. Its
heat-sensing ability helped the military flush out adversaries
hiding by night and led missiles to their targets. People
trapped in burning buildings, lost at sea or in snowdrifts,
could be rescued because their body temperature showed up
as thermal images. So far, so dramatic, but when the
technology was released into the public domain, 1960s
physicians leapt on thermography’s potential as an equally
potent life-saver in the medical sphere: cancerous tissues
emit more infra-red heat than healthy tissue, so here, it
seemed, was a surefire way of detecting tumours.
Zeal, unfortunately, ran ahead of clinical trials, which at the
time were carried out using ex-military and industrial
equipment. Thermography fell out of favour for many years
but good ideas find their own right time: in the past decade
thermography scanning has been re-introduced and refined
in tune with greater understanding of physiology and
advances in computer technology. It is now routinely used in
many areas of mainstream medicine (including
rheumatology, neurology, pain clinics and vascular-related
dysfunction). But so far it’s been most enthusiastically
embraced by the holistic health world, where its value as an
extra diagnostic tool for breast disease is seen as groundbreaking:
“It seems to spot active pre-cancerous breast signs
some six to eight years before any palpable lump appears.”
Thermography’s key asset is that it seems to spot active
pre-cancerous breast signs some six to eight years before
any palpable lump appears. This may well be in time for
wise patients to alter their lifestyle and so modify their
health, reversing the earliest changes. Speedy (the whole
procedure is over in 15 minutes), safe (there’s no exposure
to radiation) thermography is also non-invasive (so there’s
no unpleasant compression and the patient sits in a small
cosy room several feet from the scanner). So could
thermography be the new secret weapon in the battle
against breast cancer? Could it help women avoid
unnecessary mammograms and reduce exposure to harmful
radiation? Could it lead the way beyond screening
mammography which, on its own, only detects breast
disease that is already well developed enough to be seen
with x-ray? We already know that thermography works for
young women where mammography is contra-indicated
because their breast tissue is too dense to “read”. Given the
sharp rise in breast cases among younger women, this
simple screening system would be hot news indeed.
The picture – for young women especially – looks good, and
women would naturally wish thermography to take over
from mammography because it is so simple, painless and
radiation free. But Dr Peter Leando, founder and Managing
Director of Meditherm, the US firm producing high specificity
medical thermal scanners cautions against seeing
thermography as a stand-alone diagnostic miracle:
“Thermography is very much an extra, not an alternative
breast screening tool” he explains, “and I stress that we are
not in competition with mammography or taking on the
same job. Thermography works best in clinical evaluation as
an adjunct to mammography and ultrasound: a study at the
Ville Marie Institute in Canada found thermography to have
an 83 per cent detection rate as opposed to mammography’s
84 per cent. When combined, however the two services
reached 95 per cent accuracy.”
“The real purpose is to establish a base line – a thermal fingerprint.”
A thermal scan can provide additional information about the
body, but it does a different job from mammogram or
ultrasound which test structure and anatomy. Thermography
is a test, instead, of function and physiology and its
overriding purpose in specialist breast screening, says Peter
“is to monitor breast physiology and track changes over
time. A first study is not really designed to identify any
suspicious findings (though of course any patient would
immediately be referred to her physician for further clinical
investigation if worrying signs did emerge). The real purpose
is to establish a base line – a thermal fingerprint, if you like,
of the breast physiology that is normal for that particular
patient. Everyone has a vascular structure and anatomy
that’s particular to them, so what we are trying to establish
in every case is whether this thermal fingerprint is stable, so
we re-scan after the first three months to monitor for
changes that might give concern. Thereafter women are
followed up annually.”
All thermologists – the medical doctors trained to “read”
thermal scans just as radiologists read the x-ray pictures
radiographers have taken – are highly trained to look for
patterns particular to various breast conditions. These may
present as asymmetry – where the colour pattern differs in
one breast from the other – though repeat monitoring could
also evaluate this as normal for that particular woman.
“Comparing right side to left, and different areas of the
breast,” says Peter “we are looking for temperature
differentials and particularly patterns that may be
suspicious. But even if they do change over time, these
differences could also relate to fibrocystic changes, and
thermal ‘hotspots’ could simply reflect nerve irritation.”
Thermography, Peter points out, is not the appropriate firstline
service for any woman with known breast cancer:
“Mammography is more accurate for later stage cancer or
for anyone with a palpable lump, although the thermal
image can help pinpoint where the cancer is most active,
and therefore act as a useful guide for more targeted
mammography. Thermography only enables us to look at
the activity of that lump and see if it’s very vascular,
indicating angiogenesis or an active blood supply “feeding”
the tumour.
“Thermal scanning can’t give the information a mammogram provides in terms of size, density and order of the lump.”
Thermal scanning can’t give the information a mammogram
provides in terms of size, density and order of the lump. It
doesn’t provide what pathology can; it’s purely a test of
physiology. It can’t assess whether a lump is attached to the
surrounding tissue, if it’s rough or smooth, filled with fluid or
a denser, more solid mass. So much is involved in a
diagnosis of cancer. But when thermography does produce
positive findings, it justifies the more invasive tests and it
does give mammography something to look for and so aids
detection.
Thermography really comes into its own as preventative
screening before a woman ever has a scare or is called for
routine NHS mammography at 50. Although the thermal
scan colour images produced look very straightforward,
most women wanting the bottom line about breast health
would not immediately grasp what they are seeing: “What
the thermal image reflects” Peter explains, “is skin blood
flow. We don’t see any organs, any depth into the body or
any conducted heat from deeper structures or underlying
inflammation. Any thermal patterns we do see reflect the
body’s surface temperature as a neural response to
whatever is going on beneath, which could be inflammation,
lymph congestion or angiogenesis. Thermography works
because the skin, as an organ, is totally under the control of
sympathetic nerve function and thermography provides a
snapshot of the body’s response on the skin surface to any
disease or injury.” For young women who are wisely healthconscious
or, at the other end of the spectrum, concerned
about the effects of lifestyle habits like smoking or drinking,
thermography clearly fills a gap in the standard diagnostic
screening process.
As it’s non-invasive, patients can self-refer, yet come away
with a report that then becomes part of their medical record.
If thermography shows cause for concern, then it’s helpful
for a young woman to have something tangible to show her
doctor, who might otherwise dismiss her as one of the
worried well. Peter Leando says his thermography service
regularly picks up patients where a slight change registers
during the three months between initial scan and follow up.
“Sometimes mammography is negative nonetheless, and it
can take up to another year before what we first identify
becomes dense enough for mammography to identify. It
also takes quite a long time before biopsy can verify the
finding because you have to have some physical calcification
or cell growth to get a needle into.”
“Most women in this waiting state would rather not sit back and do
nothing. ‘
Most women in this waiting state would rather not sit back
and do nothing. And those wishing to do all they can to help
themselves, find their way to holistic health practitioners like
Dr Shamim Daya in Harley Street. Shamim (who explains
that she left general practice because “there was too much
emphasis on symptomatic treatment and not enough on the
root cause of the disease process”) will see the situation as a
wake-up call for any such patient in her care:
“I ask a lot of questions about women’s lifestyle and
generally find that they urgently need to clean up their act –
to cut out toxic drinks, drink more water, improve their diet,
introduce an exercise programme. The aim is to minimise
the toxic load that is primarily affecting the liver and
creating lymph congestion. For slightly older women in the
perimenopause, hormone imbalances increase stress on the
body. It’s common to find that these women have a
mouthful of mercury fillings, which also increases the toxic
load. If the lymph congestion is pronounced, I would
prescribe some herbal/homeopathic ‘drainage’ remedies as
well as suggesting that she drank more water and took
exercise. I’d ask ‘Have you done a bowel cleanse with herbal
capsules recently?’ This multi-factorial approach is intended
to get toxic waste out of your system as quickly as possible –
that’s what the breasts are trying to tell me.”
Shamim regularly sees women in their twenties who are
already at risk from smoking and drinking habits that put a
strain on key organs including the liver. Her message to
them cuts straight to the chase: “Please don’t wait till your
thirties, when you have a family and a drastic diagnosis like
breast cancer is the last thing you need.” She is quietly
confident that indications of early breast damage can be
reversed, “although in my experience thermography doesn’t
pick up a problem that will go away on its own. That’s why
we monitor. The importance of follow-up scanning is to
check for the progress of disease or its reversal, provided
my recommendations are followed. If things aren’t
improving as we would hope, then it may be necessary to
take a more aggressive approach to reduce the toxic load,
adding in specialist infrared saunas, correcting any
underlying hormonal imbalances using bio-identical (natural)
hormones and carefully supervised removal of mercury
fillings together with liver-supporting remedies.
“We can only advise and leave the responsibility to them.”
“Obviously we can’t force women to change – we can only
advise and leave the responsibility to them. Thermography
is a great tool for giving women choices and for many it’s a
great motivator for change. My resident thermographer
suggested screening to her own daughter, who seemed
impervious to warnings about booze and fags. Motivated by
her aunt’s recent breast cancer diagnosis, this young woman
came along – and was shocked enough by what she saw on
screen to change her lifestyle almost overnight.”
Thus far the NHS shows no sign of embracing thermography
So, sadly, almost all thermographic breast screening is paid
for privately: “But it’s no more expensive than a takeaway
coffee a day” says Dr Daya “We charge £185 for the first
scan, including a three month follow up. An annual scan is
£150 thereafter.” Sherrill Sellman, (one of icon’s Icons and
author of Hormone Heresy) has described the thermal
scanner as “the most neglected piece of apparatus for
female wellbeing”. Cost wise, it is relatively modest – around
£20,000 would buy a local Health Authority the whole kit –
camera, scanner computer, all the relevant software plus
training for two technicians. You could say that
thermography also has the royal seal of approval, having
been used to scan the four elegant legs of the late Queen
Mother’s racehorses at Lambourn, Berks! Thermal imaging is
very good for pain assessment and for picking up nerve
damage and muscle atrophy.
However promising, the future of thermography in twolegged
health will take its time to unfold. “Medical
developments are always very, very slow” says Peter. “But
breast screening will hopefully progress to include more
physiological assessment and a combined approach using
the different techniques for optimum results and early
detection.” Of the 600 Meditherm scanners worldwide, about
half are used predominantly in breast screening – 200 of
them in the US. In the first year of thermal scanning, one in
30 women presents with positive findings across the age
range from 25-75. That’s one more woman who can seek
early help and thank thermography for providing an extra
weapon in the war against cancer.
Examples
One
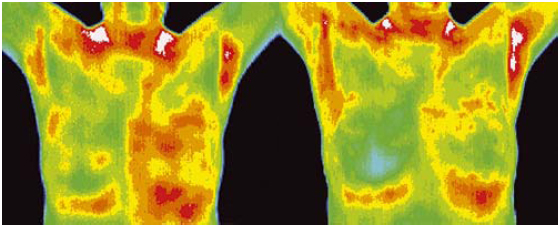
This 57 year old patient had her first scan last year. The
result was worrying so we asked for an urgent report.
Further investigation found that she was in need of natural
hormone support; she had a mouthful of mercury fillings,
metal toxicity in her liver and a sluggish lymph system
round the breasts. There was no lump to feel; ultrasound
and mammograms were negative.Yet something was
brewing that in five years or more could have become a
lump. Here we had a star patient, who was very
responsive and embarked pro-actively on a six month
restorative health programme. A year on you can see a
classic recovery. She feels great – and relieved.
Two
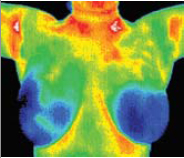
This young woman in her twenties has relatively
healthy looking breasts.
Three
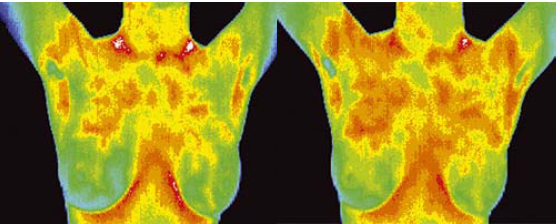
This young woman in her twenties shows lymph congestion
in both breasts which seemed more marked in her three
month follow up scans, prompting her to quit smoking and
drinking.
The images illustrating this feature were taken with a
Meditherm, Med2000 scanner.
Contact
Dr Peter Leando’s website address is:
www.meditherm.com.
Dr Shamim Daya BM DRCOG works
from the Wholistic Medical Centre, 57 Harley St, London,
W1G 8QS; Tel: 07000 388 388
Website:www.wholisticmedical.co.uk.


